 You think you’re doing a good job taking care of your oral health by brushing twice a day and flossing regularly. So it’s quite a shock to hear at your bi-yearly dental checkup that you have gingivitis or gum disease. If gingivitis isn’t treated it can turn into inflammation around the tooth, or periodontitis. This is when the gum pulls away from the tooth forming pockets where bacteria can gather and become infected.
Risk factors for gum disease include:
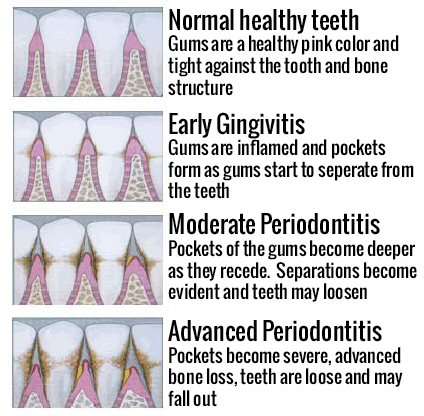
You think you’re doing a good job taking care of your oral health by brushing twice a day and flossing regularly. So it’s quite a shock to hear at your bi-yearly dental checkup that you have gingivitis or gum disease. If gingivitis isn’t treated it can turn into inflammation around the tooth, or periodontitis. This is when the gum pulls away from the tooth forming pockets where bacteria can gather and become infected.
Risk factors for gum disease include:
- Smoking.
- Diabetes.
- Certain medications.
- Hormonal changes.
- Genetics.
Symptoms of gum disease include:
- Loose teeth.
- Teeth that look “longer.”
- Changes in gums including bleeding, swelling or redness.
- Gums which have receded or pockets that have formed around the tooth.
- Chronic bad breath that isn’t controlled with mouthwash or breath spray.
During your dental exam if your dentist or hygienist suspects gum disease, you will be asked about personal habits such as smoking and alcohol consumption. Your gums will be closely inspected and if pockets have formed, a miniature ruler called a probe will be used to measure the depth of each area. X-Rays may be taken to see if any bone loss has occurred.
Treatment of gum disease includes:
- Top priority is to control any active infection.
- Deep cleaning called scaling and root planing may be necessary. Scaling removes tarter from the tooth and below and around the gum line while planing removing irregular areas when germs and bacteria can gather.
- Either OTC or prescription medications maybe prescribed to control bacteria growth.
- Dental surgery is a possibility depending on the severity or if the above measures don’t stop the inflammation.
Concerned you may have gingivitis? Please schedule an appointment with Ellis Dental today.
